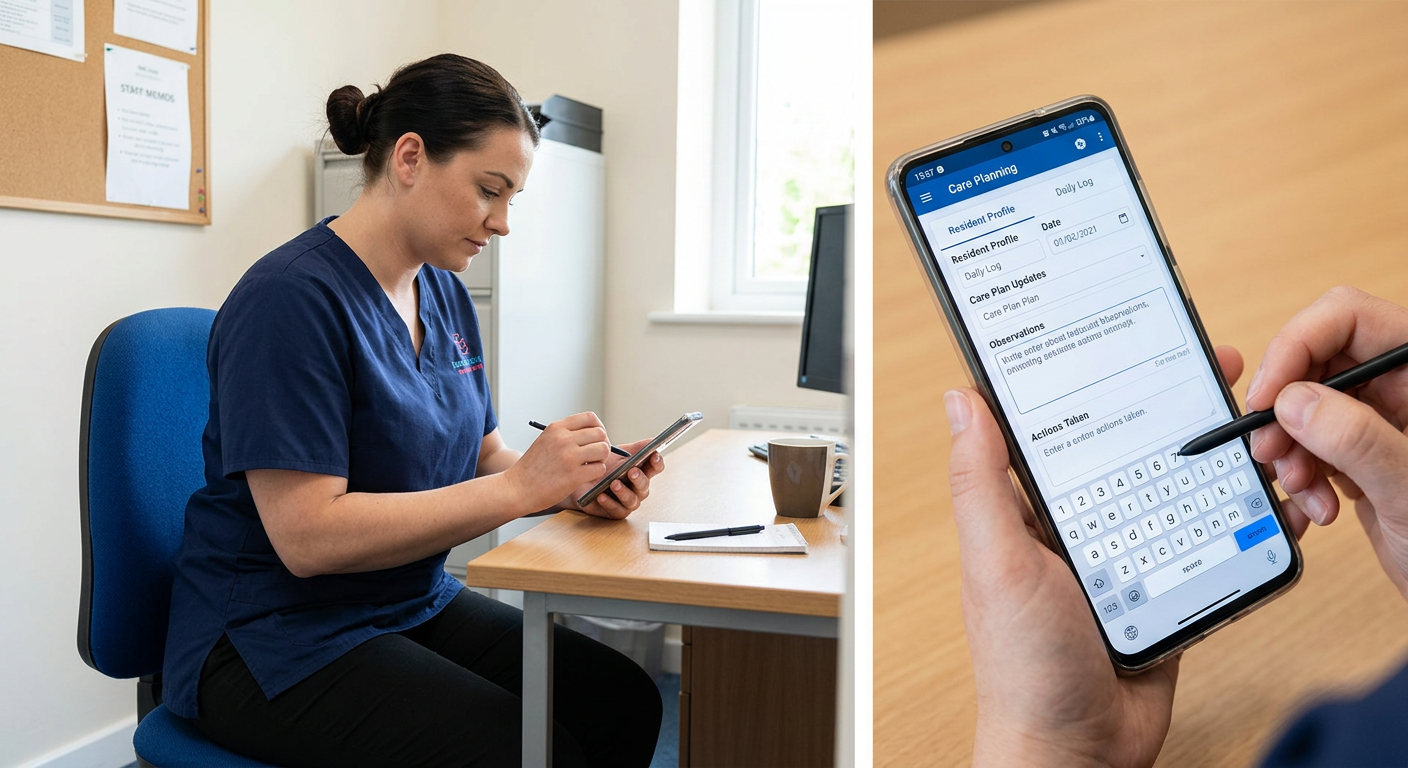
Somewhere in a care home near you, there is a care plan that hasn’t been updated in six weeks. It sits in a lever arch folder, behind a plastic divider, in a filing cabinet that smells faintly of instant coffee. The resident it describes has changed considerably since it was written. The staff who care for them have not read it recently. And when the CQC inspector arrives, everyone will scramble.
This is not a hypothetical. It is the lived reality of a sector that has been told, repeatedly and with increasing urgency, to go digital and has done so unevenly, reluctantly, and in many cases, inadequately.
The Adoption Gap Nobody Wants to Admit
Electronic care planning software has been commercially available to UK adult social care providers for well over a decade. Platforms such as Person Centred Software, Nourish, and Carely have matured significantly. The evidence base for digital care records, reduced medication errors, faster information retrieval, better audit trails, is no longer thin. And yet, according to NHS England’s own digital maturity assessments, a substantial proportion of care homes are still operating on paper or hybrid systems that offer the worst of both worlds.
The question worth asking is not whether electronic care planning software works. It does. The question is why adoption remains so patchy, and what that patchiness is actually costing residents.
The Quality Problem Hidden Inside the Technology Problem
Here is the uncomfortable truth that the sector’s digital evangelists tend to gloss over: switching from paper to electronic care planning does not automatically improve the quality of care plans. It improves their accessibility, their auditability, and their legibility. But a poor care plan entered into a tablet is still a poor care plan.
The risk, and it is a real one, is that providers invest in care planning software, complete the implementation, tick the digital transformation box, and then discover that the underlying quality of person-centred documentation has not improved at all. The template has changed. The thinking has not.
This matters because care planning software is only as valuable as the clinical and personal information it contains. A system that prompts staff to record preferences, risks, goals, and outcomes is only useful if staff have the time, training, and confidence to do so meaningfully. In a sector where the average care worker is managing multiple residents, working under significant time pressure, and may have received minimal training on the software itself, that is a significant ask.
Where the Market Has Got to, and Where It Hasn’t
The leading electronic care planning platforms have invested heavily in usability over the past few years. Mobile-first interfaces, voice-to-text recording, offline functionality, and integration with eMAR systems have all reduced the friction of digital documentation. The best platforms now feel genuinely designed for the care environment rather than adapted from healthcare IT systems built for hospitals.
But the market is fragmented. Smaller providers, particularly those running one or two homes, are often still on legacy systems, or on entry-level platforms that lack the integration capabilities needed to connect care planning with medicines management, incident reporting, and family communication. The result is a patchwork of disconnected tools that creates its own administrative burden.
Meanwhile, the larger group operators have moved decisively toward integrated platforms, and the gap between their digital capability and that of independent providers is widening. This is not just a technology story. It is a market structure story, and it has implications for how regulators, commissioners, and integrated care systems think about digital investment in the sector.
The Regulatory Pressure Is Real, But Misdirected
CQC’s single assessment framework places significant weight on evidence of person-centred care, and electronic care records are increasingly the medium through which that evidence is presented. Inspectors expect to see contemporaneous, detailed, and accessible documentation. Paper systems make this harder to demonstrate, not because the care is worse, but because the evidence trail is thinner.
This creates a perverse incentive: providers adopt electronic care planning primarily to satisfy inspection requirements rather than to improve care quality. The software becomes a compliance tool rather than a care tool. And when that happens, the potential of the technology to surface patterns, flag deterioration, support better decision-making, goes largely unrealised.
The sector needs a more honest conversation about what electronic care planning is actually for. Not just audit trails and inspection readiness. Not just reducing the risk of lost paperwork. But genuinely better, more responsive, more person-centred care, delivered by staff who understand the system, trust it, and have the time to use it properly.
What Good Looks Like
The providers getting the most from electronic care planning software share a few characteristics. They have invested in proper implementation, not just installation. They have trained staff not just on how to use the system, but on why good care documentation matters. They have built review cycles into their governance structures so that care plans are live documents, not static records. And they have chosen platforms that integrate with the rest of their digital infrastructure rather than sitting in isolation.
None of this is complicated. All of it requires sustained leadership attention and a willingness to treat digital care planning as a clinical and operational priority, not an IT project.
The lever arch folder is not going away because a tablet arrived. It goes away when the culture around documentation changes, and that is a leadership challenge, not a technology one.